You are here: Professional
Professional
Contact Dermatitis is Common and Costly
Allergen exposure is influenced by climate, occupation, cultural habits, and regulations. The prevalence of contact allergy against specific allergens differs among countries as a result of changes and developments in surrounding environments and societies. (Thyssen et al 2007) In the United States, estimates of prevalence range from 5% to 50%, depending on population and defining criteria. According to a 2005 report by The Society for Investigative Dermatology and The American Academy of Dermatology, contact dermatitis is associated with more than 9 million physician office visits and as many as 10% of all dermatology clinic visits. Treating contact dermatitis costs approximately $1.4 billion annually, with significant losses (~$500 million) attributed to missed workdays and low productivity. (Bickers et al. 2006) In the UK, occupational contact dermatitis is the most frequently reported occupational skin disease in developed countries and accounts for between 70% and 90% of all reported cases of occupational skin disease. The annual population incidence of occupational contact dermatitis ranges from an estimated 5.7 to 101 cases per 100,000 workers per year. The most reliable studies estimate the incidence to be between 11 and 86 cases per 100 000 workers per year. (Nicholson et al. 2010) Experts believe these numbers may underestimate the impact of contact dermatitis.
Allergic or Irritant Contact Dermatitis?
Although irritant contact dermatitis is thought to be more common, recent studies suggest that allergic contact dermatitis may be responsible for nearly half of dermatitis cases, especially when work related. (Templet et al., 2004; Kucenic and Belsito, 2002) The two major diagnoses of contact dermatitis are irritant (ICD) and allergic (ACD) contact dermatitis. ICD is a non-specific inflammatory dermatosis, primarily caused by the toxicity of chemicals on the skin cells, hence, triggering inflammation by activation of the innate immune system. ACD, however, corresponds to a delayed-type hypersensitivity response and the skin inflammation is mediated by antigen-specific T cells. (Nosbaum et al. 2009)
| Allergic Contact Dermatitis | Irritant Contact Dermatitis | |
| Immune Reaction | T-cell mediated; Localized, but may spread beyond contact site | No immune system involvement; Inflammation at contact site |
| Most Common Sources | Nickel, fragrance components, rubber processing chemicals, neomycin, preservatives, cobalt and potassium chromate | Detergents, acids, alkalis, oils, solvents, or exposure to abrasive, caustic or wet environments |
| Onset | Begins within hours or days of exposure | Begins within minutes or hours of exposure |
| Typical Presenting Symptoms | Pruritis, papules, vesicles, edema, fissures, erythema, and oozing May spread beyond contact site | Skin dryness, fissuring and thickening; edema and erythema Distribution localized to contact site |
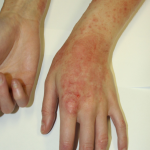
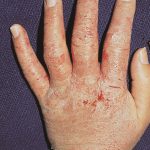
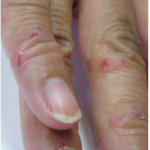
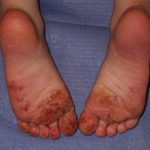
Allergic contact dermatitis
In already sensitized individuals, this immunologic response is elicited by contact with a specific allergen or closely related chemical. Symptoms typically manifest 24 to 72 hours after allergen exposure, vary in intensity and often include itching and vesiculation.
More than 3,000 chemicals are reportedly capable of causing allergic contact dermatitis but relatively few allergens account for most cases. These common allergens form the basis of diagnostic patch testing that is used to differentiate allergic from irritant contact dermatitis.
Irritant contact dermatitis:
This non-specific inflammatory condition develops after skin is exposed to substances that are physically, chemically or mechanically traumatizing. Symptoms are usually confined to the area of contact, recur with additional irritant exposure and may be difficult to distinguish from allergic contact dermatitis.
Why Patch Test?
Patch testing is a simple bioassay that helps diagnose and identify causative agent(s) in persistent contact dermatitis. Even experienced dermatologists can miss 20% to 80% of contact allergies when using history alone. (Fischer and Maibach 1990) Patient symptoms, history and physical exam are rarely sufficient. Patch test results can provide crucial information that identifies the offending allergen(s). (Lachapelle and Maibach 2009)
Patient interviews show that patch testing has a positive impact, with a perceived improvement in symptoms. (Paul et al., 1995) Patients learn to identify and avoid allergens, protect their skin from irritants and other allergens, and use therapies appropriately.
Early diagnosis and patient education are associated with improved prognosis, and may be more valuable than job changes. (Cahill et al., 2004; Woo et al., 2003) In a retrospective study of 270 patients with allergic contact dermatitis, patient disease duration after contact allergen testing and treatment was half that of patients treated without testing. (Diepgen 2008; Rajagopalan et al., 1998) Not surprisingly, 84% of patients felt patch testing was worthwhile.
An earlier study reported that symptom duration decreased by half in patients with allergic contact dermatitis who were patch tested.
Patients can suffer with contact dermatitis for up to 40 years. (Holness and Mace, 2001; Bickers et al. 2006) Unresolved dermatitis costs patients in terms of multiple doctor visits, prescriptions, over-the-counter medicaments, as well as lost time and productivity. The prognosis for these patients with persistent unresolved dermatitis is poor, and most will experience discomfort, embarrassment and other factors that diminish their quality of life. (Holness, 2001; Ayala et al., 2010)